Maximizing immigrant medical skills
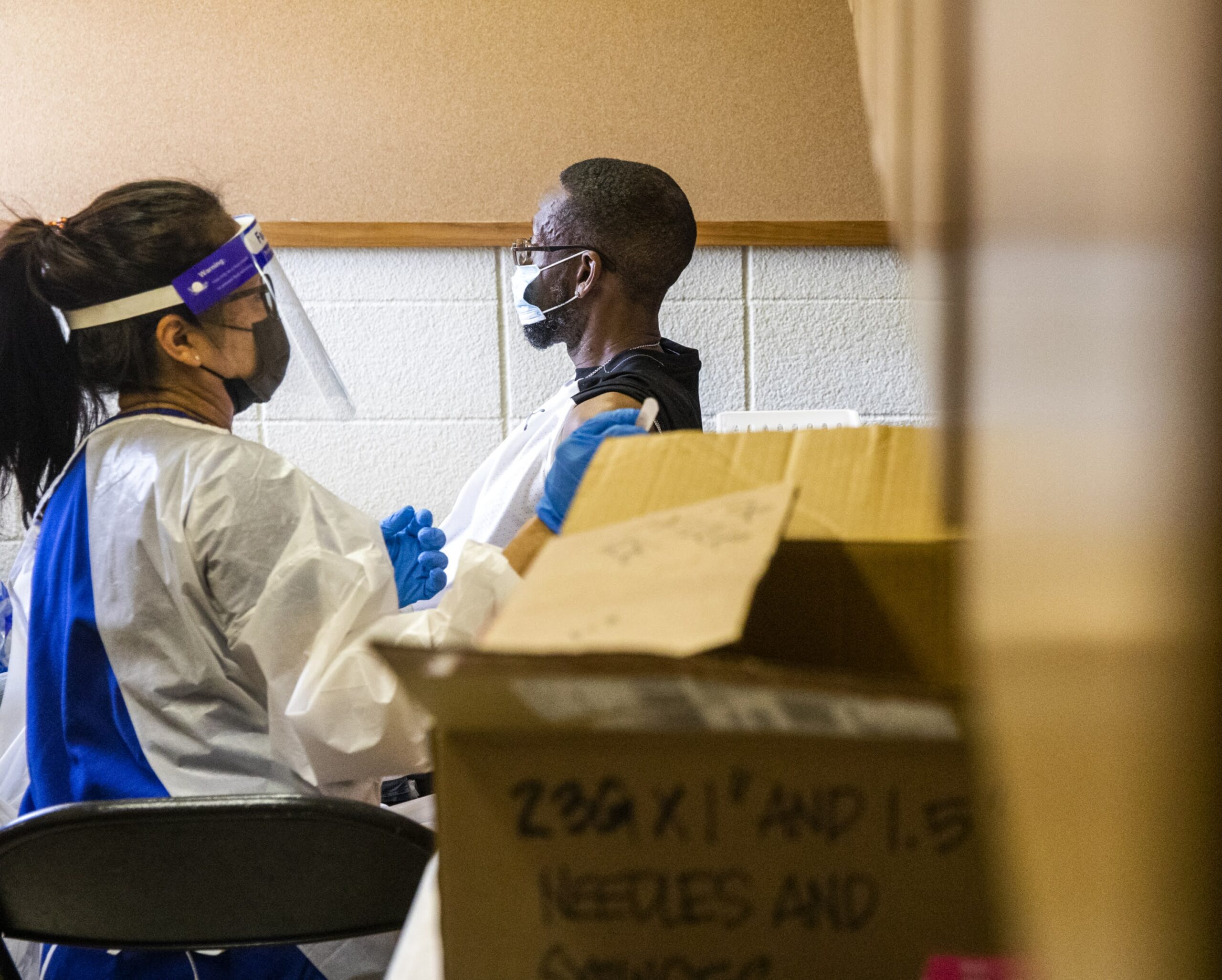
Each year, thousands of immigrants from several countries arrive in the United States. A large number of them come to Nevada, with the state planning to welcome at least 150 citizens from Afghanistan in 2021. Many new arrivals have health care backgrounds (physician, nurse, medical technician, etc.) that could potentially assist in improving medical care delivery in Clark County and even statewide.
Because medical education completed in other countries is often not recognized in the United States, additional training can be required for licensing and credentialing. A centralized and structured program that identifies, tracks, and mentors those with critical and high-demand medical skills might make this possible. The proposed program’s ultimate outcome would be to develop more healthcare professionals who can service medically underserved areas across Nevada.
There are a few organizations that would be central to such an initiative. Key among them would be Catholic Charities of Southern Nevada (CCSN), which assists new immigrants when they first arrive. During inprocessing, CSSN staff could document any healthcare training received in home countries to help identify potential candidates for developmental training.
This information would then be shared with another agency, perhaps Workforce Connections (WC), which has partnerships with employers, to include healthcare agencies. WC could then establish a licensing and/or credentialing action plan for those selected for training. The plan would detail the skills a candidate must master to obtain the necessary license or credential, where education and training would be received, and appropriate placement based on skills and community needs after training is completed.
State or federal funding would be required for potential WC staffing increases and medical education and training costs. Nonprofits and healthcare organizations might also provide support. Candidates would be expected to work during the program, but a modest stipend is recommended. (Full scholarships funded by Nevada or local governments that cover all living expenses are discouraged because of cost. If a program is enacted, efforts should be made to ensure the program and its processes do not become overly burdensome or bureaucratic or incur excessive and increasing costs.)
A two-year test period, with rigid, measurable, and objective metrics, should be sufficient time to determine whether the program is worthwhile. Quarterly concise updates (absent superfluous content) should be provided. If at the end of two years results reveal that the program has little merit, it should be discontinued — not allowed to grow and meander and become hostage to the “just one more year” syndrome as so often happens.
This is, of course, a broad outline of a program that would require many more details and the involvement of political and community leaders to establish. Leadership commitment will be imperative to create a program that has the potential to alleviate health care shortages in many communities throughout the Silver State. If successful, though, it could become a model for the nation. Nevada could lead the way.
Colonel Linnes Chester (ret.), USAF, MSC, is a former senior medical advisor to the Afghanistan National Police. He lives in Las Vegas. He is a Democrat. Dr. Babak Haidarian, M.D., was a former supervising medical translator/coordinator in Kabul, Afghanistan. He is an Independent. Neither has any paid or unpaid political or business affiliations related to the article.

